
Polycystic ovarian syndrome or PCOS is the most common hormonal abnormality in this population, affecting about 4–18% of reproductive-age women. [1] Signs and symptoms can range in severity from increased androgen production (male hormones) and altered gonadotropin secretion. These hormones can force its sufferers to deal with irregular or prolonged periods, excess body and facial hair (hirsutism), acne, and male-pattern baldness. Nothing a girl wants! Not surprisingly, these symptoms lead to increased anxiety and depression among women and even adolescents. [2] [3] [4] Still, even more devastating to some PCOS patients is the possibility of infertility and increased risk of endometrial cancer. [5] [6] [7]
If that wasn’t enough, PCOS also has metabolic characteristics leading to even more health problems, including increased risk of insulin resistance, type 2 diabetes, fatty liver disease, dyslipidemia, a prothrombotic state, and cardiovascular disease. [7] [8] As you might have guessed, PCOS is strongly associated with obesity, with prevalence of 80% amongst patients in the United States. [9]
Doctors use one of three sets of criteria to diagnose patients with PCOS [8]:

Once diagnosed, treatments vary based on individual preferences and desired fertility. Multiple pharmaceutical options are available to address specific comorbidities of PCOS, including oral contraceptives, Metformin (Glucophage), Clomiphene, Inositol, and Spironolactone. But before medication is prescribed, a crucial part of management is exercise and diet.
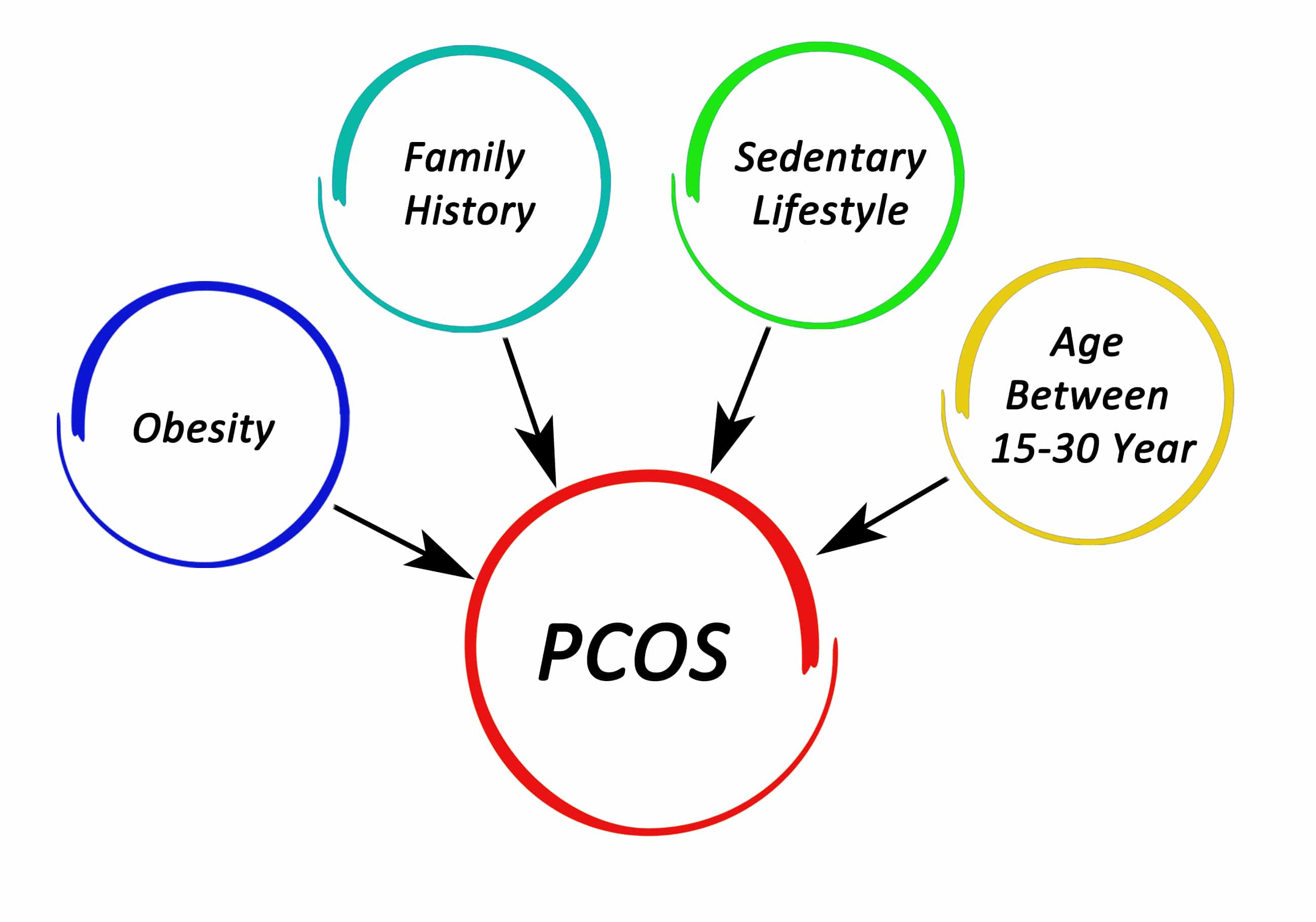
The exact cause of PCOS is still unclear, but we know there’s a substantial connection to excess weight, insulin resistance, and metabolic syndrome. [10] [11] Insulin resistance and hyperinsulinemia appear to be linked to PCOS independent of obesity. High blood levels of insulin can increase hormone stimulation in the ovaries as well as act on reproductive hormones in the brain and adrenal glands. [12] So, it would be intuitive to make dietary changes to decrease insulin levels, naturally restore insulin sensitivity, and reverse metabolic syndrome while reducing weight. This is where the ketogenic diet shines!
 Studies have shown that even without weight loss, compared to a standard diet, reducing carbohydrates in PCOS patients led to decreased fasting insulin levels, fasting glucose levels, insulin resistance, total testosterone, and cholesterol. [13] [14] Additional studies have demonstrated similar findings, in addition to weight loss, that further substantiate the benefits of a low-carbohydrate diet. [15] Specifically, the ketogenic diet has shown significant improvement in weight, reproductive hormone levels, and fasting insulin levels in women with obesity and PCOS. [16]
Studies have shown that even without weight loss, compared to a standard diet, reducing carbohydrates in PCOS patients led to decreased fasting insulin levels, fasting glucose levels, insulin resistance, total testosterone, and cholesterol. [13] [14] Additional studies have demonstrated similar findings, in addition to weight loss, that further substantiate the benefits of a low-carbohydrate diet. [15] Specifically, the ketogenic diet has shown significant improvement in weight, reproductive hormone levels, and fasting insulin levels in women with obesity and PCOS. [16]
It is evident that a ketogenic diet will reduce insulin levels and body weight, which will in turn reduce or improve symptoms of PCOS. As always, discuss with your doctor before discontinuing any medications or dietary interventions. Check out ketogenic.com’s list of keto-friendly doctors!
References
Dennett, C. C., & Simon, J. (2015). The role of polycystic ovary syndrome in reproductive and metabolic health: overview and approaches for treatment. Diabetes Spectrum, 28(2), 116-120.
Sam, S. (2007). Obesity and polycystic ovary syndrome. Obesity management, 3(2), 69-73.
Chaudhari, A. P., Mazumdar, K., & Mehta, P. D. (2018). Anxiety, depression, and quality of life in women with polycystic ovarian syndrome. Indian journal of psychological medicine, 40(3), 239.
Sadeeqa, S., Mustafa, T., & Latif, S. (2018). Polycystic ovarian syndrome–related depression in adolescent girls: A Review. Journal of pharmacy & bioallied sciences, 10(2), 55.
Blay, S. L., Aguiar, J. V. A., & Passos, I. C. (2016). Polycystic ovary syndrome and mental disorders: a systematic review and exploratory meta-analysis. Neuropsychiatric disease and treatment, 12, 2895.
Ding, D. C., Chen, W., Wang, J. H., & Lin, S. Z. (2018). Association between polycystic ovarian syndrome and endometrial, ovarian, and breast cancer: A population-based cohort study in Taiwan. Medicine, 97(39).
Randeva, H. S., Tan, B. K., Weickert, M. O., Lois, K., Nestler, J. E., Sattar, N., & Lehnert, H. (2012). Cardiometabolic aspects of the polycystic ovary syndrome. Endocrine reviews, 33(5), 812-841.
El Hayek, S., Bitar, L., Hamdar, L. H., Mirza, F. G., & Daoud, G. (2016). Poly cystic ovarian syndrome: an updated overview. Frontiers in physiology, 7, 124.
Ehrmann, D. A., Barnes, R. B., Rosenfield, R. L., Cavaghan, M. K., & Imperial, J. (1999). Prevalence of impaired glucose tolerance and diabetes in women with polycystic ovary syndrome. Diabetes care, 22(1), 141-146.
Moini, A., Javanmard, F., Eslami, B., & Aletaha, N. (2012). Prevalence of metabolic syndrome in polycystic ovarian syndrome women in a hospital of Tehran. Iranian journal of reproductive medicine, 10(2), 127.
Mandrelle, K., Kamath, M. S., Bondu, D. J., Chandy, A., Aleyamma, T. K., & George, K. (2012). Prevalence of metabolic syndrome in women with polycystic ovary syndrome attending an infertility clinic in a tertiary care hospital in south India. Journal of human reproductive sciences, 5(1), 26.
Paoli, A., Rubini, A., Volek, J. S., & Grimaldi, K. A. (2013). Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets. European journal of clinical nutrition, 67(8), 789.
Gower, B. A., Chandler‐Laney, P. C., Ovalle, F., Goree, L. L., Azziz, R., Desmond, R. A., … & Bates, G. W. (2013). Favourable metabolic effects of a eucaloric lower‐carbohydrate diet in women with PCOS. Clinical endocrinology, 79(4), 550-557.
Douglas, C. C., Gower, B. A., Darnell, B. E., Ovalle, F., Oster, R. A., & Azziz, R. (2006). Role of diet in the treatment of polycystic ovary syndrome. Fertility and sterility, 85(3), 679-688.
Phy, J. L., Pohlmeier, A. M., Cooper, J. A., Watkins, P., Spallholz, J., Harris, K. S., … & Boylan, M. (2015). Low starch/low dairy diet results in successful treatment of obesity and co-morbidities linked to polycystic ovary syndrome (PCOS).Journal of obesity & weight loss therapy, 5(2).
Mavropoulos, J. C., Yancy, W. S., Hepburn, J., & Westman, E. C. (2005). The effects of a low-carbohydrate, ketogenic diet on the polycystic ovary syndrome: a pilot study. Nutrition & metabolism, 2(1), 35.