Want to start going keto but you’re concerned about the risk of hypertension on a ketogenic diet? Let’s set the record straight with keto and blood pressure.
Blood pressure may be on your mind daily if you deal with the common struggle of trying to lower your high blood pressure. But what exactly is blood pressure? Here is the textbook definition:
“Blood pressure: the force per unit area exerted on a vessel wall by the contained blood.” [1]
Blood Pressure Explained
When the heart pumps blood, it produces blood flow. Blood pressure results when that flow is opposed by resistance. Sources of resistance to flow include blood viscosity (the thickness of the blood), blood vessel length, and blood vessel diameter (i.e., fatty plaques deposited in the artery may reduce diameter). Pressure is the greatest in the large arteries that receive the blood directly from the pumping heart.
Systolic blood pressure is the pressure in the aorta (the large artery connected to the heart) that occurs when the heart releases blood during a contraction. Systolic 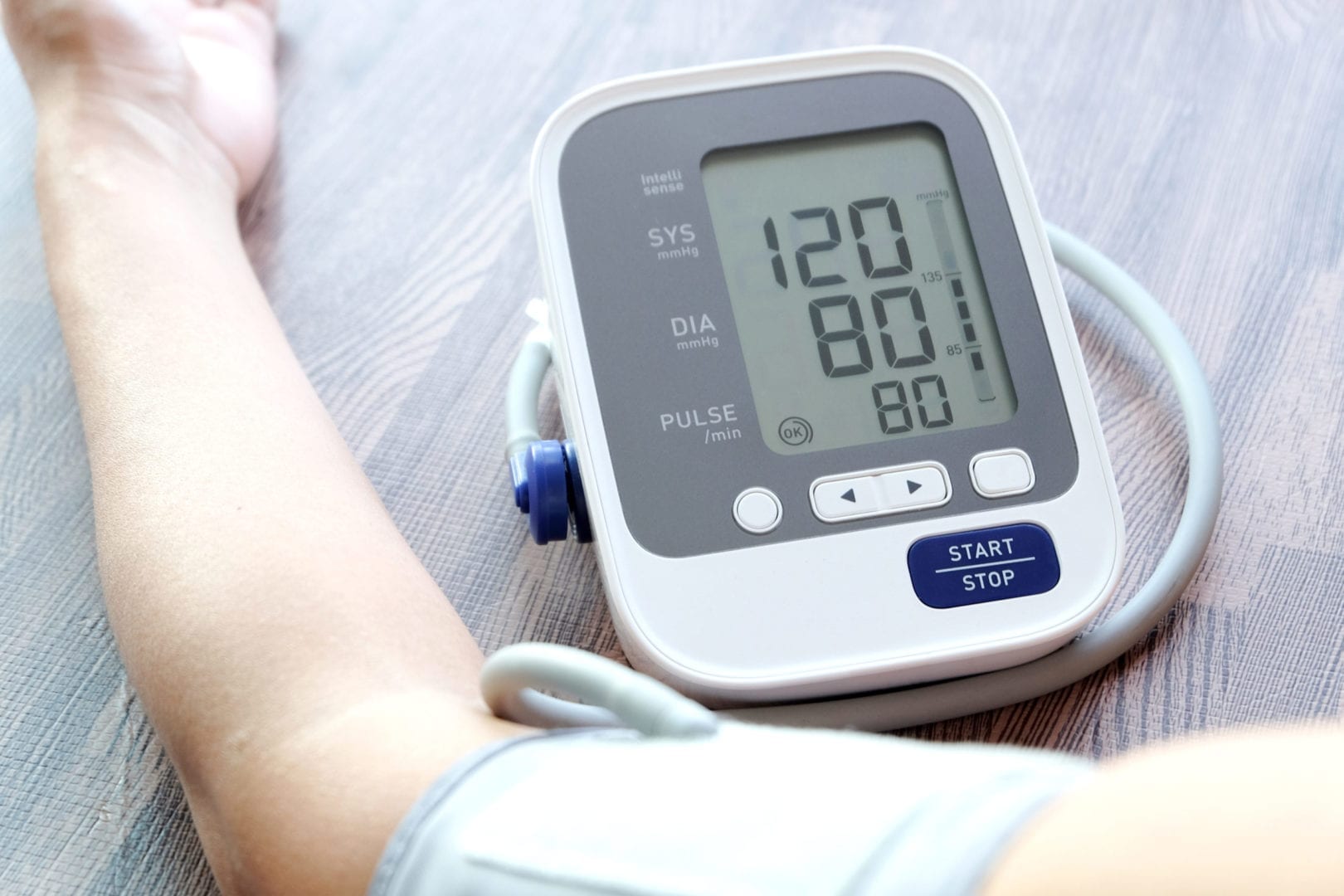 blood pressure is the highest blood pressure in the body and 120 mm Hg is considered a normal resting value in healthy adults.
blood pressure is the highest blood pressure in the body and 120 mm Hg is considered a normal resting value in healthy adults.
Diastolic blood pressure is the lowest pressure in the aorta that occurs when the heart relaxes and stops releasing blood into the vessel. 80 mm Hg is considered a normal resting diastolic blood pressure in healthy adults.
Blood pressure is less as the blood moves through the body. The gradient from high to low pressure is extremely important as it keeps the blood moving in the right direction through the body, from areas of high to areas of lower pressure. [1]
Hypertension
Hypertension occurs when blood pressure is chronically elevated and is defined as a resting systolic blood pressure >140 mm Hg or a diastolic blood pressure >90 mm Hg. Hypertension is known as the “Silent Killer”. Why? Because individuals may have hypertension for years without any symptoms or side effects. However, the many symptom-less years of elevated blood pressure results in increased strain on the heart and damaged arteries which commonly leads to serious and fatal conditions like heart failure, renal failure, and stroke.
Hypertension and Keto: Reducing Blood Pressure Through Diet
Low-carbohydrate, ketogenic diets have been examined in the research as an intervention to lower blood pressure and related variables. Research studies are mixed in their findings, as some show no change in blood pressure, [2] [3]some show a reduction in diastolic blood pressure, [4] [5] and some show a reduction in systolic blood pressure. [6] [7] [8] However, all of the studies demonstrate improved health markers that are related to blood pressure. [2] [3] [4] [5] [6] [7] [8]
For instance, keto diets have been shown to reduce the risk for plaque formation in the arteries by lowering total cholesterol, increasing the “good” HDL cholesterol, and reducing triglycerides in the circulation. [2] [3] [4] [5] [6] [7] [8] [9] [10] When plaques form in the artery from circulating cholesterol and lipids, the diameter of the artery becomes smaller which increases blood pressure. Also, diabetes and obesity are risk factors for hypertension, which may both improve after implementing a KD. [2] [3] [4] [5] [7] [8] [9] [10]
Some individuals are more genetically predisposed to higher blood pressures and should be very careful of the environmental factors that may contribute to hypertension. Individuals predisposed to hypertension include those with hypertensive parents as well as specific races such as African Americans. Environmental factors that may increase the risk for developing hypertension include poor diet, obesity, >40 years old, diabetes, high stress, and smoking. [1] The environmental factors that you can control are diet, obesity, type 2 diabetes, stress level, and smoking.
Therefore, individuals with hypertension or predisposed to hypertension may benefit in many ways by incorporating and maintaining a keto diet into their lifestyle. A KD may eliminate many of the controllable environmental factors associated with increased risk for hypertension including appropriate diet, reducing obesity and type 2 diabetes, and possibly even reducing stress level via reductions in anxiety.[11] It is important to discuss these findings with your doctor and figure out a plan to reduce chronically elevated blood pressure before more serious conditions occur.
References
Marieb, E. N., & Hoehn, K. (2013). Human anatomy & physiology. Pearson Education.
Dansinger, M. L., Gleason, J. A., Griffith, J. L., Selker, H. P., & Schaefer, E. J. (2005). Comparison of the Atkins, Ornish, Weight Watchers, and Zone diets for weight loss and heart disease risk reduction: a randomized trial. Jama, 293(1), 43-53.
Davis, N. J., Tomuta, N., Schechter, C., Isasi, C. R., Segal-Isaacson, C. J., Stein, D., … & Wylie-Rosett, J. (2009). Comparative study of the effects of a 1-year dietary intervention of a low-carbohydrate diet versus a low-fat diet on weight and glycemic control in type 2 diabetes. Diabetes care, 32(7), 1147-1152.
Foster, G. D., Wyatt, H. R., Hill, J. O., McGuckin, B. G., Brill, C., Mohammed, B. S., … & Klein, S. (2003). A randomized trial of a low-carbohydrate diet for obesity. New England Journal of Medicine, 348(21), 2082-2090.
Foster, G. D., Wyatt, H. R., Hill, J. O., Makris, A. P., Rosenbaum, D. L., Brill, C., … & Zemel, B. (2010). Weight and metabolic outcomes after 2 years on a low-carbohydrate versus low-fat diet: a randomized trial. Annals of internal medicine, 153(3), 147-157.
Iqbal, N., Vetter, M. L., Moore, R. H., Chittams, J. L., Dalton‐Bakes, C. V., Dowd, M., … & Wadden, T. A. (2010). Effects of a low‐intensity intervention that prescribed a low‐carbohydrate vs. a low‐fat diet in obese, diabetic participants. Obesity, 18(9), 1733-1738.
Gardner, C. D., Kiazand, A., Alhassan, S., Kim, S., Stafford, R. S., Balise, R. R., … & King, A. C. (2007). Comparison of the Atkins, Zone, Ornish, and LEARN diets for change in weight and related risk factors among overweight premenopausal women: the A TO Z Weight Loss Study: a randomized trial. Jama, 297(9), 969-977.
Shai, I., Schwarzfuchs, D., Henkin, Y., Shahar, D. R., Witkow, S., Greenberg, I., … & Tangi-Rozental, O. (2008). Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet. New England Journal of Medicine, 359(3), 229-241.
Brinkworth, G. D., Noakes, M., Buckley, J. D., Keogh, J. B., & Clifton, P. M. (2009). Long-term effects of a very-low-carbohydrate weight loss diet compared with an isocaloric low-fat diet after 12 mo–. The American journal of clinical nutrition, 90(1), 23-32.
Holland, A. M., Kephart, W. C., Mumford, P. W., Mobley, C. B., Lowery, R. P., Shake, J. J., … & Huggins, K. W. (2016). Effects of a ketogenic diet on adipose tissue, liver, and serum biomarkers in sedentary rats and rats that exercised via resisted voluntary wheel running. American Journal of Physiology-Regulatory, Integrative and Comparative Physiology, 311(2), R337-R351.
Ari, C., Kovács, Z., Juhasz, G., Murdun, C., Goldhagen, C. R., Koutnik, A. P., … & D’Agostino, D. P. (2017). Exogenous ketone supplements reduce anxiety-related behavior in Sprague-Dawley and Wistar Albino Glaxo/Rijswijk rats.Frontiers in molecular neuroscience, 9, 137.