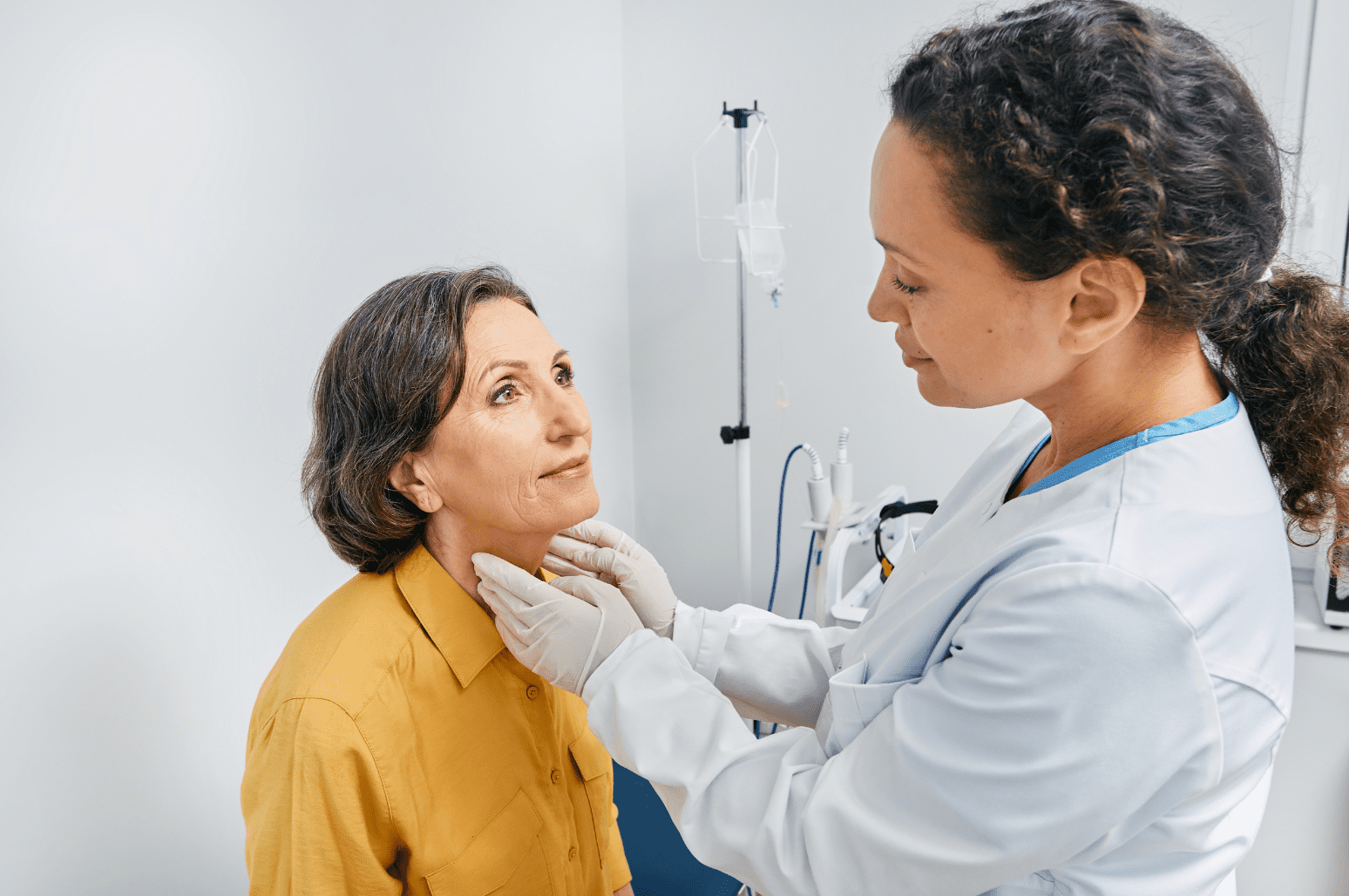
Hashimoto’s thyroiditis is the most common autoimmune disease in the world. It is also the largest cause of hypothyroid problems in the U.S. [1]
Hashimoto’s affects up to 3 percent of the population, with subclinical hypothyroidism affecting as much as 10 percent. [2] Beyond that, some 22 percent of the population experiences some form of thyroid disorder or abnormal thyroid levels. [3]
Finding dietary ways to address the symptoms of Hashimoto’s is essential because there is no cure. Even when patients are given hormone replacement, inflammatory and other chronic factors can reduce the quality of life without lifestyle and nutritional intervention.
How Does Keto Help Hashimoto’s?
The thyroid regulates metabolism and it has significant control over body weight, energy expenditure, and even body temperature. When autoimmunity kicks in, the immune system mistakenly attacks the thyroid and interferes with its normal function.
Research has found a large portion of this to be due to inflammation and targeting of thyroid hormones and antibodies. When dietary changes were made to reduce processed and high-starch carbs, like bread and pasta, the results included not only weight loss, but decreased levels of thyroid antibodies and reduced inflammation. [4] By normalizing these, a ketogenic diet can promote a decrease in overall autoimmunity and balanced thyroid health.
Another study followed the autoimmune protocol (AIP), which is a version of a Paleo diet. Lower in carbs than a traditional American diet, AIP excludes inflammatory foods like nuts, seeds, and all grains. Patients in the study didn’t have lowered antibodies, but they had demonstrated reduced inflammatory markers. [5]
It is possible that the best diet for Hashimoto’s could be a combined version of high-fat, low-carb, and the autoimmune protocol. This would effectively reduce inflammatory foods or those that can negatively impact gut health.
Concluding Thoughts
Ultimately, a keto diet isn’t detrimental to thyroid health, like many believe. More research is needed to determine keto’s overall effect on Hashimoto’s and thyroid health, but what we currently know is promising.
References
Ahmed R, Al-Shaikh S, Akhtar M. Hashimoto thyroiditis: a century later. Adv Anat Pathol. 2012 May;19(3):181-6. DOI: 10.1097/PAP.0b013e3182534868. PMID: 22498583.
Wojtas, N., Wadolowska, L., & Bandurska-Stankiewicz, E. (2019). Evaluation of Qualitative Dietary Protocol (Diet4Hashi) Application in Dietary Counseling in Hashimoto Thyroiditis: Study Protocol of a Randomized Controlled Trial. International journal of environmental research and public health, 16(23), 4841. https://doi.org/10.3390/ijerph16234841
Latina A, Gullo D, Trimarchi F, Benvenga S. Hashimoto’s thyroiditis: similar and dissimilar characteristics in neighboring areas. Possible implications for the epidemiology of thyroid cancer. PLoS One. 2013;8(3):e55450. doi: 10.1371/journal.pone.0055450. Epub 2013 Mar 18. PMID: 23526929; PMCID: PMC3601092.
Esposito, T., Lobaccaro, J. M., Esposito, M. G., Monda, V., Messina, A., Paolisso, G., Varriale, B., Monda, M., & Messina, G. (2016). Effects of low-carbohydrate diet therapy in overweight subjects with autoimmune thyroiditis: possible synergism with ChREBP. Drug design, development and therapy, 10, 2939–2946. https://doi.org/10.2147/DDDT.S106440
Abbott, R. D., Sadowski, A., & Alt, A. G. (2019). Efficacy of the Autoimmune Protocol Diet as Part of a Multi-disciplinary, Supported Lifestyle Intervention for Hashimoto’s Thyroiditis. Cureus, 11(4), e4556. https://doi.org/10.7759/cureus.4556