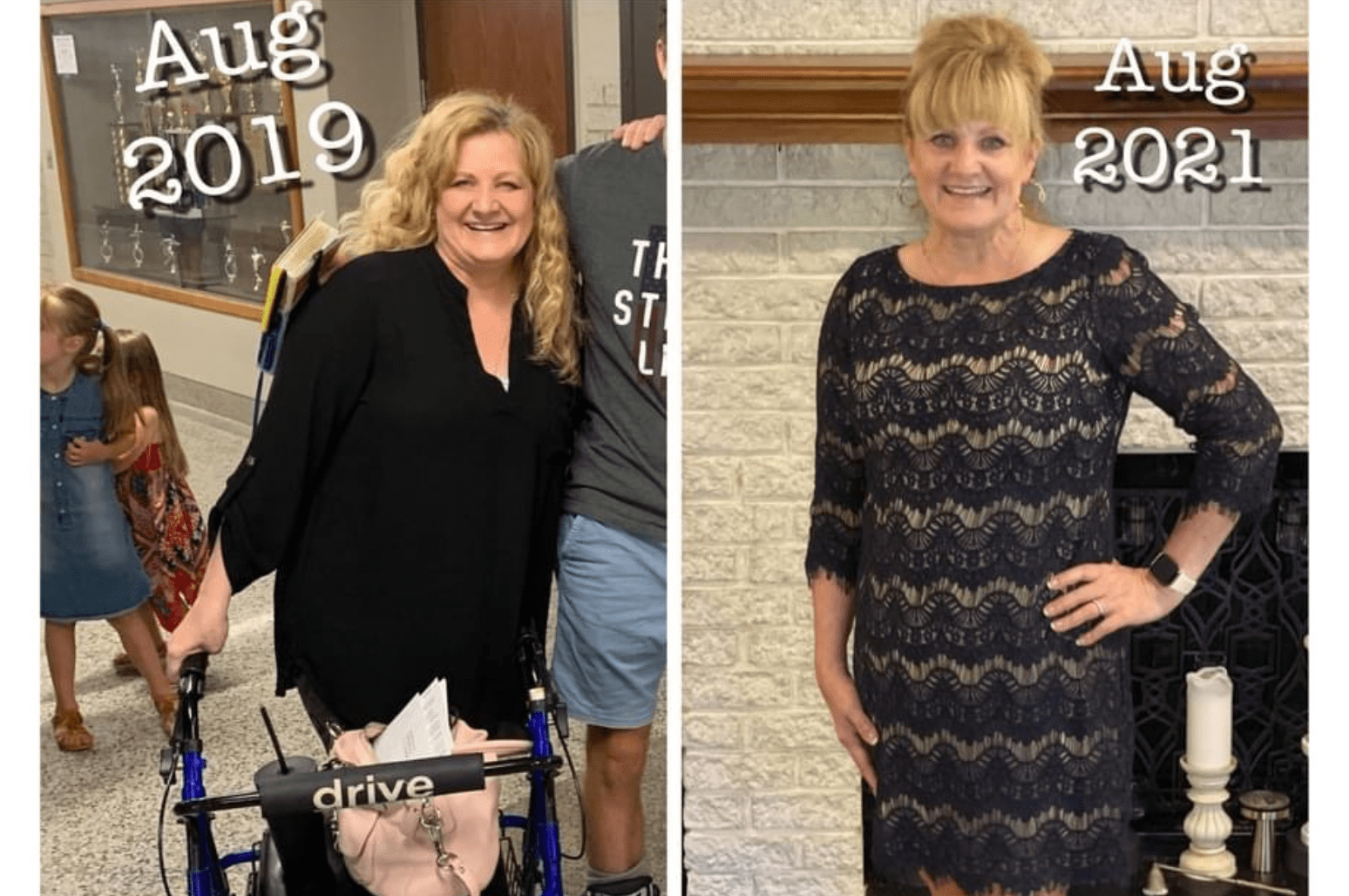Chasing Mental Clarity: How to Improve Focus and Cognition

It’s no secret that going keto can improve focus, cognition, and mental clarity, and mounting scientific evidence and anecdotal stories corroborate this. For a long time, this therapeutic way of eating has been effectively used to treat various mental health and brain conditions, such as Alzheimer’s, Parkinson’s, epilepsy, bipolar disorder, and depression. As an inspiring example, check out Natasha’s personal story here at Ketogenic.com.
A surprising 264 million people globally deal with depression. [1] Countless people are also suffering from brain fog — mild to severe episodes of mental confusion. Going keto is one way to help manage these problems and enhance mood and cognitive functioning.
Keto and Cognitive Functioning: Delving into the Research
Experts emphasize the connection between diet and how well your brain works. A key culprit in impairing brain function might actually be excess consumption of refined carbohydrates, such as grain-based flours and cereals, fruit juice, and sugars and syrups.
Another key player is refined industrial vegetable oils, such as canola oil. Highly refined carbohydrates and industrial oils might promote oxidation and inflammation. [2] [3] [4]
Going keto requires ditching these refined carbohydrates, which could lower inflammation, and consequently improve cognition.
When it comes to vegetable oils, you could try to avoid products that contain these vegetable oils and choose to cook with healthier oils at home, such as coconut oil and animal fats like tallow.

A ketogenic diet has been widely studied for a range of neurological and psychiatric conditions. For example, one case study of a 70-year-old woman with lifelong schizophrenia, including daily visual and auditory hallucinations, showed a complete resolution of symptoms in just eight days on a ketogenic diet. The woman continued the ketogenic diet, and a one-year follow-up confirmed the hallucinations hadn’t returned. [5]
One study assessed ten women with schizophrenia following a ketogenic diet for two weeks alongside standard treatment of medication and electroconvulsive therapy (ECT). The study revealed a significant reduction in symptoms. One week after the women went back to their usual diets, symptoms came back. [6]
Some of the strongest scientific research on the ketogenic diet and brain disorders is on epilepsy. Implementing a therapeutic ketogenic diet for epilepsy has been studied for near a century. Bipolar disorder and epilepsy share several features. [7]
Alzheimer’s disease involves a decline in glucose (carbohydrate) metabolism in certain parts of the brain. This decline in glucose metabolism might also be involved with other neurological problems. To simplify: some areas of the brain can’t use glucose for fuel as efficiently as they need to. When this ability to use glucose as a fuel is compromised, the brain needs another source of fuel.
This is where ketones come in. In Alzheimer’s patients, mild ketosis has been shown to enhance cognitive function. [8]
The ketogenic diet might also help cognition in other ways, such as improving nerve cell signaling and increasing blood flow to specific parts of the brain.
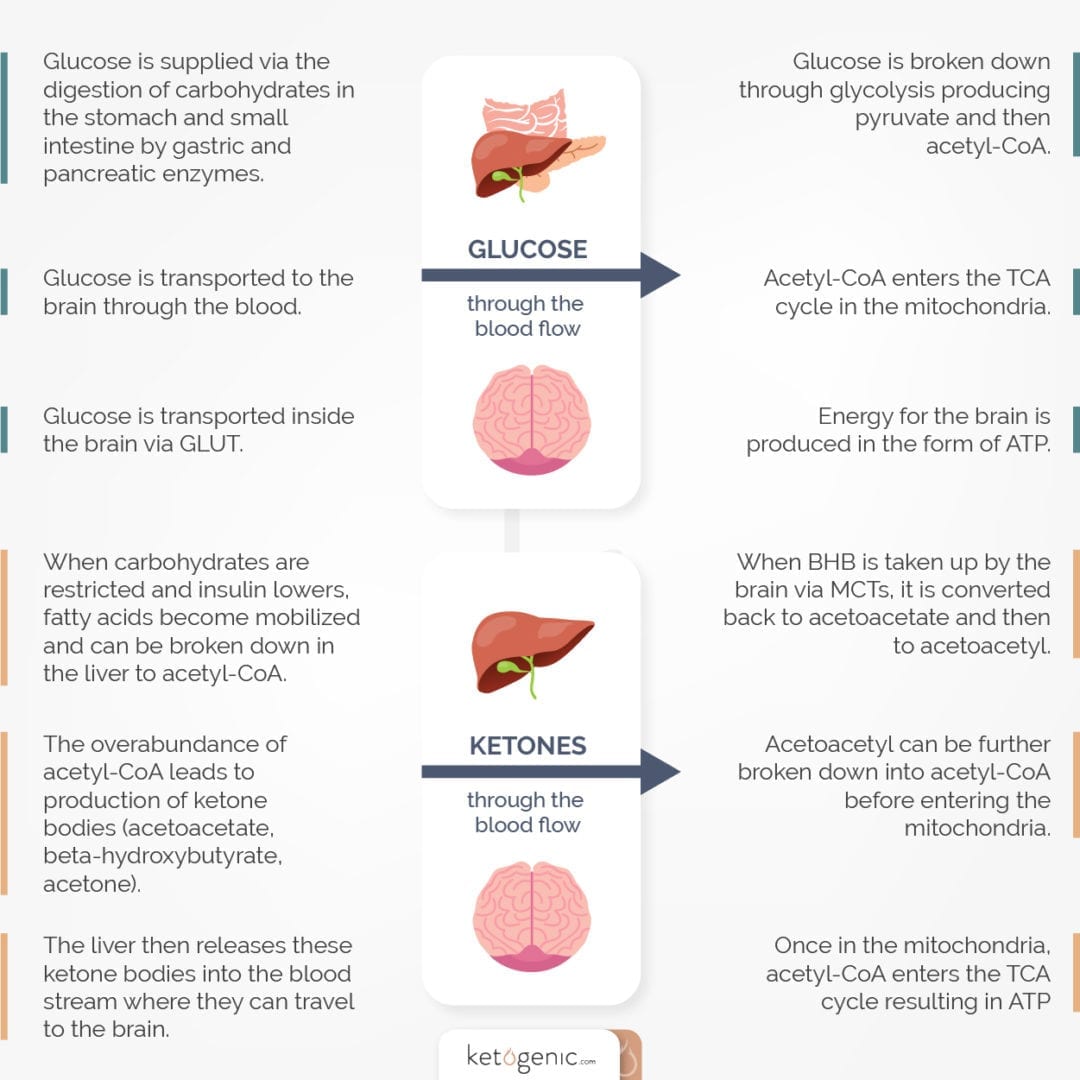
Two Fuels: Ketones Vs. Glucose
The brain can use two fuels: ketones and glucose. When you drop your carbohydrate (glucose) consumption on keto, your body switches to using ketones. Your liver produces ketones from the breakdown of fatty acids derived from the fat in your diet or the fat stored in your body. Ketones are an alternative energy source that can cross the blood-brain barrier and provide energy for your brain in the absence of glucose.
Your body obtains glucose by breaking down the carbohydrates you eat.
While a small number of your cells need glucose, even if you don’t eat any carbohydrates, your liver can produce glucose from its own breakdown products or from the breakdown of proteins or lipids (fats). This process is called gluconeogenesis. This is why protein and fats are necessary for survival, but carbohydrates aren’t. [10]
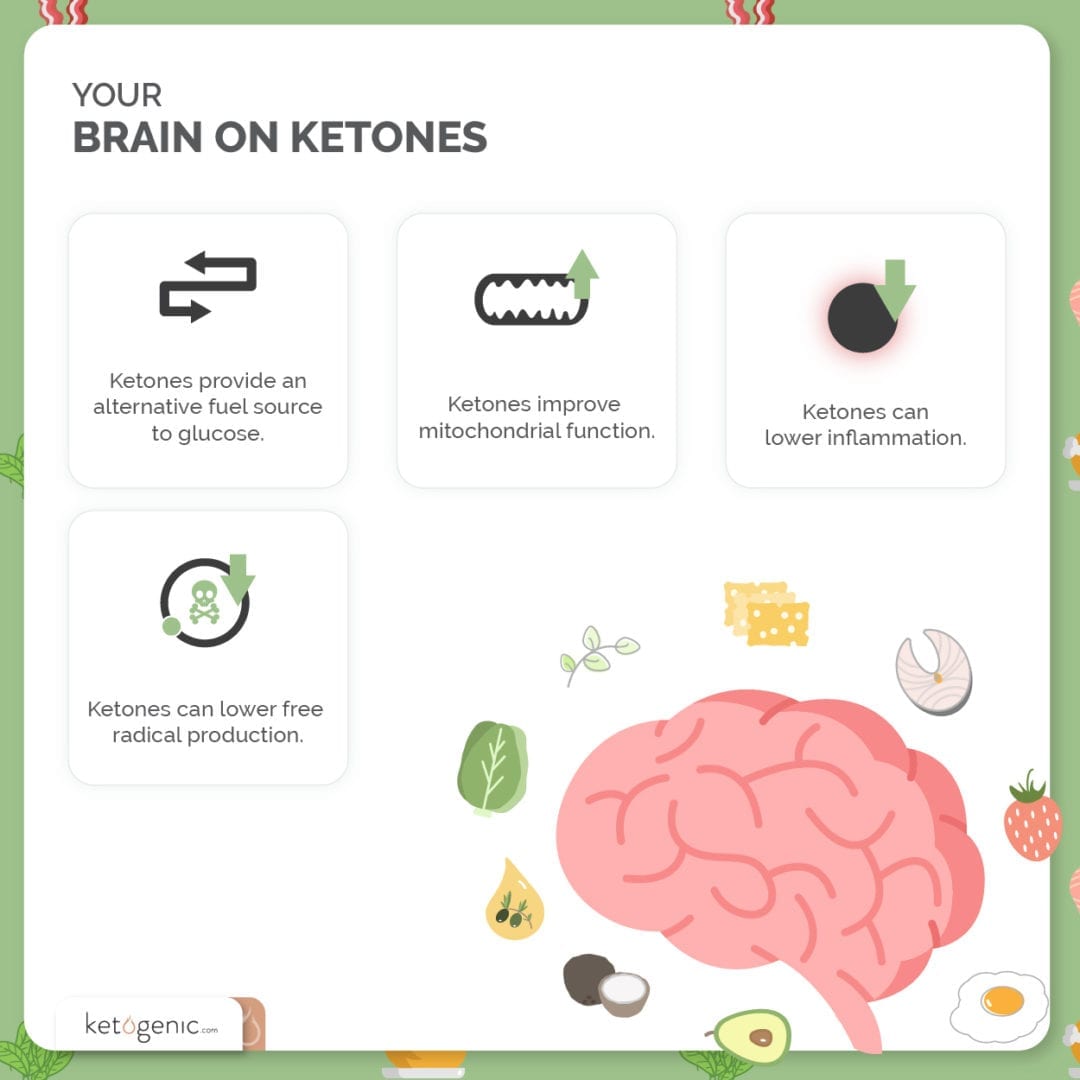
Ketones as a fuel for the brain might boost nerve cell growth factors and energy production, reduce brain inflammation, and strengthen the signal sent between nerve synapses. [11] [9]
The Blood Sugar Rollercoaster
Keto has been shown to help manage blood sugar, including in those with diabetes. Managing blood sugar can improve mood. Blood sugar levels have a drastic effect on mood, and both very high and very low blood sugar usually come along with negative alterations in mood.
You might have experienced this yourself if you’ve become down or irritable after going too long without eating or if you’ve eaten way too much sugar and experienced a surge of energy followed by a foggy crash.
The key to avoiding this is stepping off the blood sugar rollercoaster and keeping your levels under control. If you avoid the blood sugar spikes and crashes that come with the high-carb diet, research shows it could also boost your mood and reduce fatigue. A huge number of people struggle with blood sugar control when they eat carbs in excess. High carb consumption is common with the standard American diet.

What About Wheat?
Most people end up ditching a lot of wheat-based products on a keto diet because most wheat-based products are high-carb and off-limits. Still, those dealing with mental health disorders might benefit from ditching wheat altogether, including hidden sources. Of all the high-carbohydrate foods, wheat might be the most significant for mental health.
Almost fifty years ago, researchers suggested there could be a link between symptoms in some people with schizophrenia and wheat consumption. [12]
Celiac disease is a condition with an established association to neurologic and psychiatric conditions.
Six out of every one hundred people might also have non-celiac gluten sensitivity, which could spark psychiatric symptoms. The main proteins discussed when it comes to wheat are the gluten proteins. Many people report feeling much better after going gluten-free. [13] [14] [15]
Fortunately, if you do go gluten-free, you have plenty of tasty alternatives to work with, such as almond and coconut flour and keto nut-flour bread!
In Conclusion
You might find going keto diminishes or alleviates your psychiatric or neurological symptoms. This delicious and nutritious diet plan can be life-changing. Peruse the recipes section here at Ketogenic.com for fun ideas!
Some people can wean off and completely stop their medications on a ketogenic diet. It’s always best to speak with your physician or health care practitioner before making any dietary changes.
Keto can be beneficial for neurological and mental health conditions. To summarize, keto acts on the brain by:
- Improving blood sugar regulation
- Protecting against oxidative stress and inflammation
- Increasing blood flow to some regions of the brain
- Changing brain energy metabolism
If you’re already following a ketogenic diet and you’re looking for other methods to boost your cognition, even more, you could try:
- Getting plenty of sleep
- Replenishing electrolytes (such as adding an electrolyte powder to your drinks and eating more nutrient-rich foods!)
- MCT oil
- Yoga and exercise
- Meditation and stress relief
- Nature and sunlight
- Reading and brain exercises (such as games)
Has a Ketogenic Diet Improved Your Cognition?
Has a ketogenic diet enhanced your mental function? Are you using keto to help manage a neurological or mental health condition? Find a supportive community here at Ketogenic.com and share your story!
References
World Health Organization (WHO). Depression. Depression (who.int)
Aeberli, I., Gerber, P. A., Hochuli, M., Kohler, S., Haile, S. R., Gouni-Berthold, I., Berthold, H. K., Spinas, G. A., & Berneis, K. (2011). Low to moderate sugar-sweetened beverage consumption impairs glucose and lipid metabolism and promotes inflammation in healthy young men: A randomized controlled trial. American Journal of Clinical Nutrition, 94(2), 479-485. DOI: 10.3945/ajcn.111.013540
Sottero, B., Gargiulo, S., Russo, I., Barale, C., Poli, G., & Cavalot, F. (2015). Postprandial dysmetabolism and oxidative stress in type 2 diabetes: Pathogenic mechanisms and therapeutic strategies. Med Res Rev, 35(5), 968-1031. DOI: 10.1002/med.21349
Patterson, E., Wall, R., Fitzgerald, G. F., Ross, R. P., & Stanton, C. (2012). Health implications of high dietary omega-6 polyunsaturated fatty acids. J Nutr, Metab, DOI: 10.1155/2012/539426
Kraft, B. D., & Westman, E. C. (2009). Schizophrenia, gluten, and low-carbohydrate, ketogenic diets: A case report and review of the literature. Nutr Metab (Lond), DOI: 10.1186/1743-7075-6-10
Pacheco, A., Easterling, W. S., & Pryer, M. W. (1965). A pilot study of the ketogenic diet in schizophrenia. American Journal of Psychiatry, 121(11), 1110.
Wheless, J. W. (2008). History of the ketogenic diet. Epilepsia, 49(Suppl. 8), 3-5. History of the ketogenic diet (wiley.com)
Henderson, S. T., Vogel, J. L., Barr, L. J., Garvin, F., Jones, J. J., & Constantini, L. C. (2009). Study of the ketogenic agent AC-1202 in mild to moderate Alzheimer’s disease: A randomized, double-blind, placebo-controlled, multicenter trial. Nutr Metab (Lond), DOI: 10.1186/1743-7075-6-31
Courchesne-Loyer, A., Croteau, E., Castellano, C-A., St-Pierre, V., Hennebelle, M., & Cunnane, S. C. (2017). Inverse relationship between brain glucose and ketone metabolism in adults during short-term moderate dietary ketosis: A dual tracer quantitative positron emission tomography study. J Cereb Blood Flow Metab, 37(7), 2485-2493. DOI: 10.1177/0271678X16669366
Adeva-Andany, M. M., Gonzalez-Lucan, M., Donapetry-Garcia, C., Fernandez-Fernandez, C., & Ameneiros-Rodriguez, E. (2016). Glycogen metabolism in humans. BBA Clinical, 5, 85-100. https://doi.org/10.1016/j.bbacli.2016.02.001
Koppel, S. J., & Swerdlow, R. H. (2018). Neuroketotherapeutics: A modern review of a century-old therapy. Neurochem Int, DOI: 10.1016/j.neuint.2017.05.019
Dohan, F. C. (1966). Wheat ‘consumption’ and hospital admissions for schizophrenia during World War II: A preliminary report. American Journal of Clinical Nutrition, 18(1), 7-10. DOI: 10.1093/ajcn/18.1.7
Jackson, J. R., Eaton, W. W., Cascella, N. G., Fasano, A., & Kelly, D. L. (2013). Neurologic and psychiatric manifestations of celiac disease and gluten sensitivity. Psychiatr Q, 83(1), 91-102. DOI: 10.1007/s11126-011-9186-y
Igbinedion, S. O., Ansari, J., Vasikaran, A., Gavins, F. N., Jordan, P., Boktor, M., & Alexander, J. S. (2017). Non-celiac gluten sensitivity: All wheat attack is not celiac. World J Gastroenterol, 23(40), 7201-7210. DOI: 10.3748/wjg.v23.i40.7201
Porcelli, B., Verdino, V., Bossini, L., Terzuoli, L., & Fagiolini, A. (2014). Celiac and non-celiac gluten sensitivity: A review on the association with schizophrenia and mood disorders. Auto Immun Highlights, 5(2), 55-61. DOI: 10.1007/s13317-014-0064-0